Depending on a patient’s symptoms and the degree to which they experience these symptoms, any number of examinations may be done to determine the direction in which we proceed. A typical diagnosis may involve:
- A physical examination
- Blood tests
- Imaging tests
- Nerve function tests
- Electromyography
Another important aspect when diagnosing neuropathy is classifying the kind of neuropathy a patient has. There are four classification categories that we look for when determining a diagnosis and treatment plan:
Diabetic Neuropathies
Diabetes is one of the most common causes of peripheral neuropathy in the U.S and will occur in over 50 percent of diabetics. Symptoms are most common in the feet and legs, and neuropathy rates are highest for those who have had the disease for 25 years.
Idiopathic Compression Neuropathies
Approximately 30 to 40 percent of neuropathy cases are idiopathic, meaning no known cause. Just because the neuropathy is of an undetermined cause does not mean it cannot be treated. In fact, our expertise at The Institute for Advanced Reconstruction is in assessing complex cases and finding treatment solutions regardless of the cause.
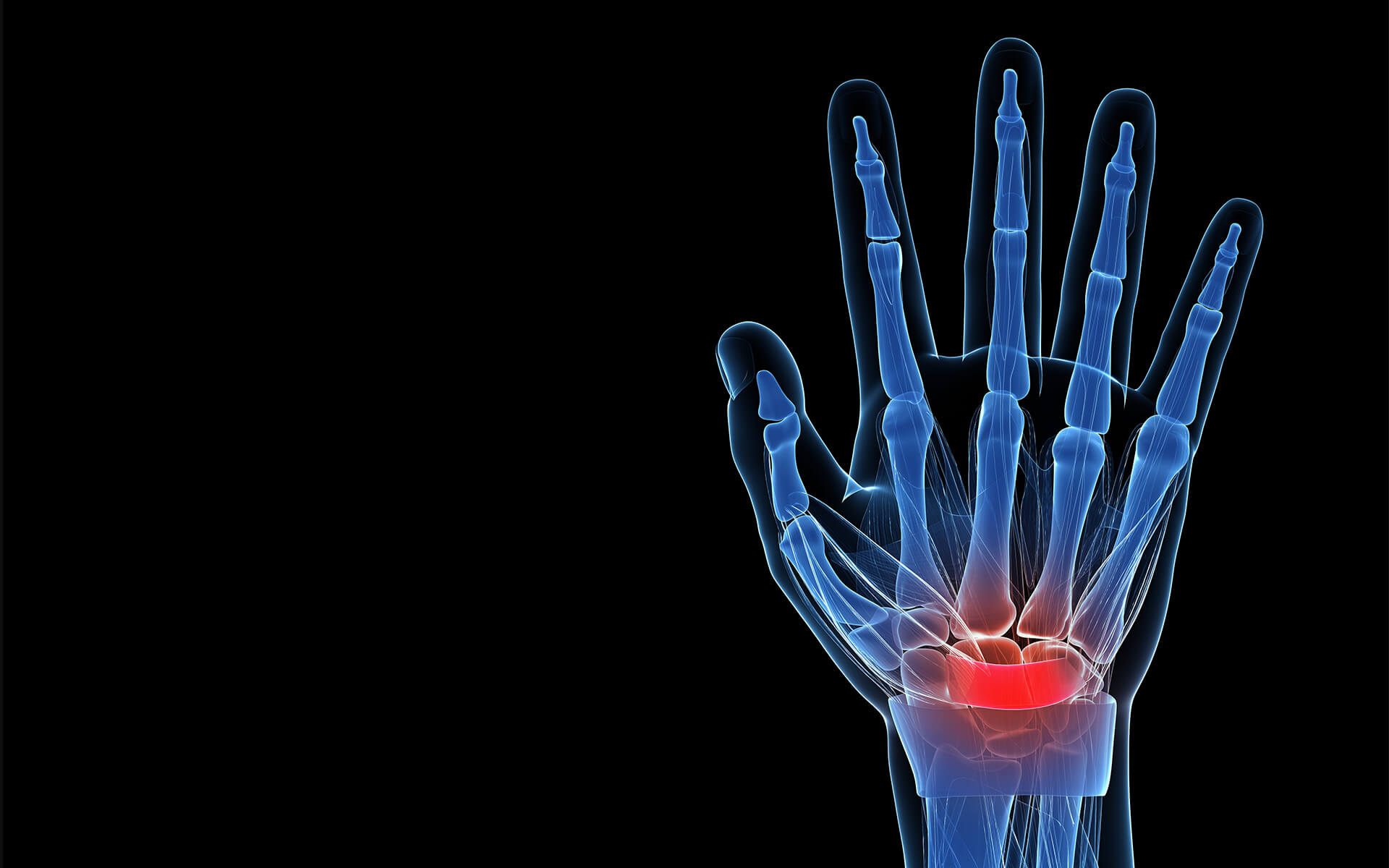
Compression Neuropathies
Also known as entrapment neuropathy, and often referred to as a pinched nerve, this is the most common cause of mononeuropathy. Carpal tunnel syndrome is the most widely known compression neuropathy, followed by ulnar neuropathy at the elbow and compression of the peroneal nerve at the fibular head, which causes foot drop.
Drug-induced Neuropathy
In some people, medications may cause nerve damage that results in a loss of sensation or movement in part of the body. For example, neuropathy is a common side effect of chemotherapy. Peripheral neuropathy will often go away if the problematic drug is changed or discontinued or if the dose is reduced. In extreme cases, however, the nerve damage may be permanent.

-1.jpg)



