Summarize This Article:
Summarize This Article:

October is Breast Cancer Awareness Month. Breast Cancer Awareness month is an amazing cause that many companies and groups of people partake in initiatives for to raise awareness and fundraise for breast cancer research and treatments. Breast cancer is something that affects us all- even if you haven’t been directly affected yourself, you most likely know a breast cancer survivor in your family, friends or colleagues. For many years, the medical community has been united in the fight against breast cancer.
As cancer treatment options continue to improve, cancer survivor rates also continue to increase. But, what happens after a patient wins the “fight”? What should they be aware of following breast cancer treatment? Several major networks, news publications, and medical resources fail to mention what can happen following breast cancer treatment. They focus on the fact that their patient “beat” breast cancer, but many patients aren’t properly prepared about the long-term complications they could potentially face following breast cancer treatment. Three of these conditions are lymphedema, chemotherapy-induced neuropathy, and radiation-induced brachial plexopathy.
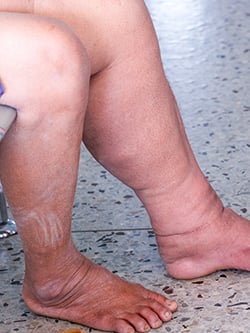
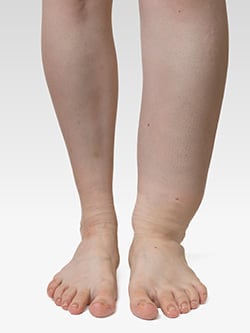
Lymphedema is a chronic condition that often manifests as an abnormal buildup of fluid, causing swelling, most commonly in the arms or legs. This swelling may be present from birth or develop without a known reason. Lymphedema can also develop after radiation or certain cancer-related surgeries. Initially reversible, lymphedema typically progresses to irreversible, restricting range of motion and limiting activities of daily living. Secondary lymphedema can occur in the arms when lymph nodes from the underarm are damaged or removed, which oftentimes occurs during mastectomies or lumpectomies. This was the case for 51-year-old Karen B., a veterinarian from Vermont. Karen was diagnosed with breast cancer, had a bilateral mastectomy and developed lymphedema in the right arm. She underwent breast reconstruction in her home state with tissue expanders but suffered multiple infections and failed salvage attempts.
Karen then found Dr. Russell Ashinoff, who was able to perform a combined surgery to reconstruct her right breast and treat her lymphedema. Dr. Ashinoff performed DIEP flap breast reconstruction, a lymph node transfer and lymphaticovenous anastomosis. During a lymph node transfer procedure, lymph nodes are harvested from one area of the body and transferred to the area of lymph node deficiency, improving drainage of the affected limb. The nodes are mapped prior to surgery to avoid causing lymphedema at the donor site. Lymphaticovenous anastomosis (LVA) is an advanced microsurgical procedure designed to create alternate routes for excess lymphatic fluid to exit the affected limb.
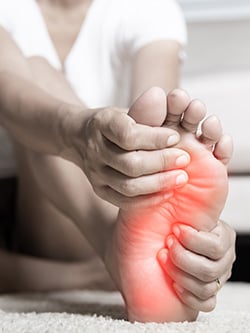
Another debilitating condition that many patients are unaware of is chemotherapy-induced neuropathy. Many potential side effects from chemotherapy are explained when breast cancer patients undergo treatment, but neuropathy is seldom one of them. Neuropathy is nerve pain that results from damage to or compression of the nerves outside the spinal cord and brain. Symptoms include pain, numbness, tingling and weakness of the affected extremity. According to the American Cancer Society, chemotherapy drugs spread through the whole body, and certain types of chemotherapy can damage different nerves. Up to 30% of cancer patients will experience persistent neuropathy long after completion of treatment. Symptoms tend to start farthest away from the head but move closer over time. In most cases, people will notice chemo-induced peripheral neuropathy (CIPN) symptoms in the feet, then later on in the hands.
Dr. Michael Rose was able to provide long-term symptom relief to neuropathy patient, Debbie P. following surgical treatment. He performed nerve decompression surgery to release the pressure on the affected nerve, which in turn relieves the pain and numbness associated with neuropathy. Debbie had breast cancer, a double mastectomy, and completed multiple rounds of chemotherapy. She didn’t react well to chemotherapy and was in and out of the hospital multiple times with infections. About a month after stopping chemotherapy, she noticed her feet were tingling. As time went on, the tingling was accompanied by intense pain, so bad she couldn’t even wear shoes besides slippers or UGG boots. Today, Debbie is pain-free.
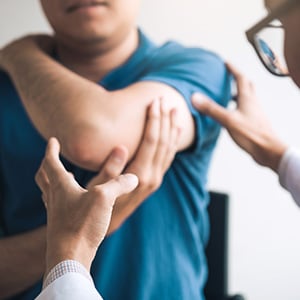
Radiation, like chemotherapy, may also result in injury to nerves, but symptoms may not appear until years after treatment. 61-year-old Lori A., patient of Dr. Andrew Elkwood, was diagnosed with breast cancer and treated with radiation. Years after her cancer treatment, she experienced a decreased range of motion and inability to complete tasks due to weakness in her hand and arm. Lori had developed radiation-induced brachial plexopathy.
The brachial plexus is a large, complex bundle of nerves in the shoulder. Nearly all signals that go from the brain to the upper arm and chest pass through the brachial plexus. When a person sustains injury to the shoulder, neck or arm, the nerves of the brachial plexus can also sustain damage, which can cause loss of sensation, paralysis of the arm, or chronic pain. The nerves of the brachial plexus may also be damaged by exposure to infectious agents, chemotherapy, or radiation from radiation therapy. Lori had undergone radiation in 1996, which is why she was scared by the symptoms she was experiencing 22 years later. Fortunately, Dr. Elkwood was able to utilize microsurgical techniques to repair the brachial plexus, eliminating her pain and symptoms and restoring function to Lori’s left arm.
These little-known conditions that may result from breast cancer treatment can often be overlooked. Patients should be educated on all options and potential complications that may occur at some point in their lifetime. While rare, there are other patients out there fighting the same battle, even after beating breast cancer. Educating patients on these aforementioned conditions and the treatment options available is paramount in a successful post-cancer journey.

%20after%20cancer%20treatment_.webp)