Summarize This Article:
Summarize This Article:

Lymphedema is a lifelong condition affecting millions worldwide. The symptoms can be vague or similar to other conditions, many providers do not have experience diagnosing or treating lymphedema, and given that there is no definitive test for diagnosis, many individuals find themselves suffering without any real answers.
There is no cure for lymphedema; however, specific treatments can alleviate many symptoms and improve quality of life. But before pursuing a treatment plan, it's essential to understand what exactly lymphedema is and is not. If you’re wondering, “how does lymphedema affect everyday life?” We have answers.
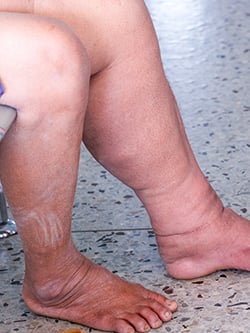
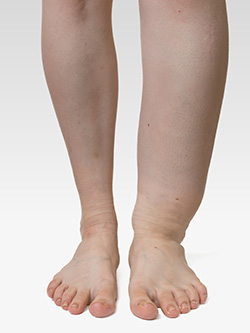 Lymphedema is an accumulation of lymph fluid in the body's tissues. It usually occurs in the arms and legs but can also occur in other body parts. Symptoms include:
Lymphedema is an accumulation of lymph fluid in the body's tissues. It usually occurs in the arms and legs but can also occur in other body parts. Symptoms include:
Lymphedema is generally not life-threatening, but it can lead to complications if left untreated or poorly managed, such as:
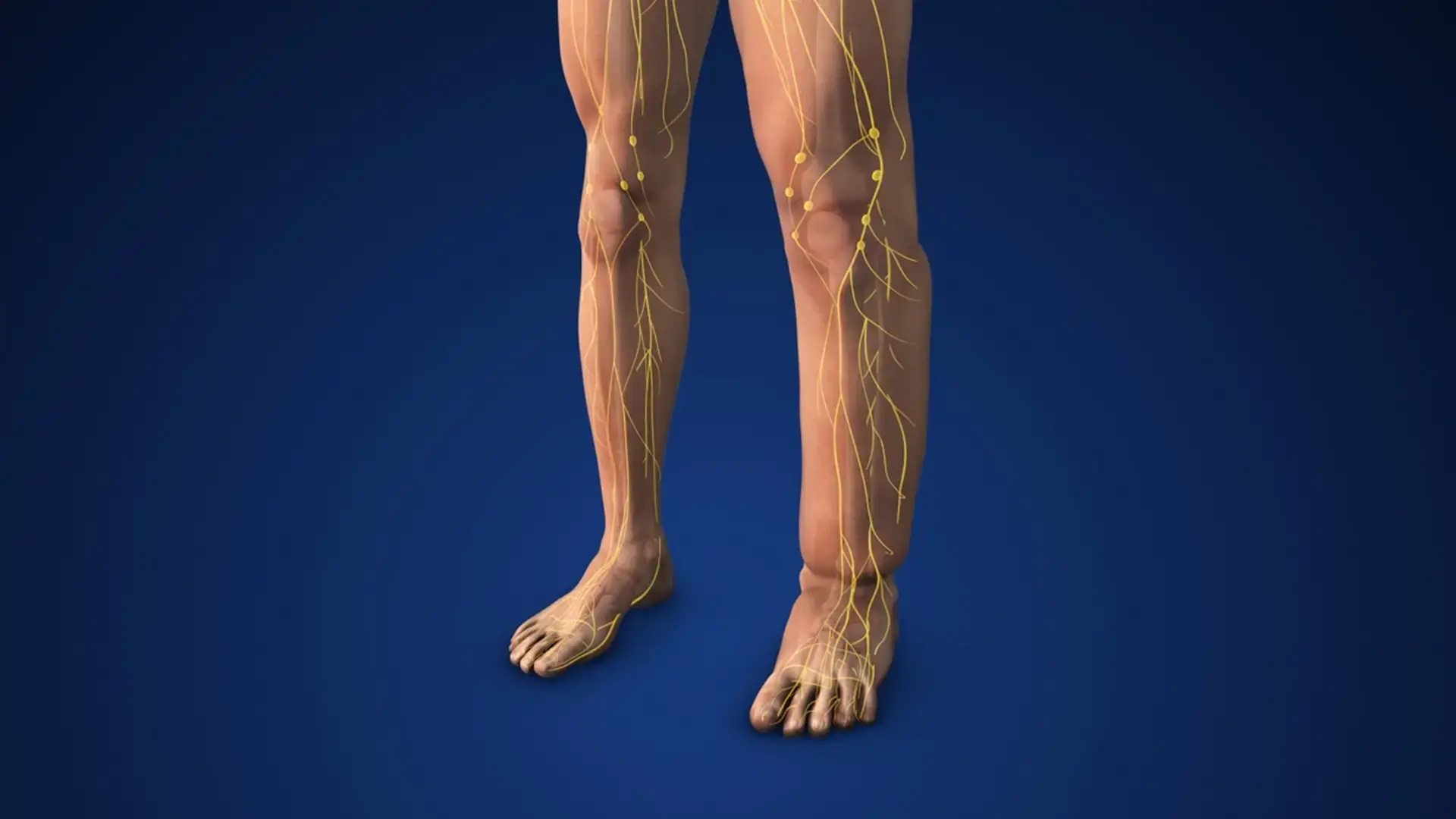
Lymphedema can be caused by various factors that prevent proper drainage of lymphatic fluid from areas of the body where it is present. The condition is classified by two types:
Primary lymphedema is a rare genetic condition that is present at birth or develops later in life due to a genetic mutation that affects the development or function of the lymphatic system.
Secondary lymphedema, on the other hand, is a more common form of lymphedema that occurs as a result of damage to the lymphatic system, including:
Lymphedema can occur at any age, but it typically develops in adulthood, usually around the age of 45 or older. Those with certain genetic conditions, such as Milroy and Meige disease, may also be predisposed to developing primary congenital lymphedema later in life.
Anyone who has had damage to their lymphatic system due to surgery, radiation therapy, or other treatments may be at risk for developing this condition. People who are obese or have a chronic skin infection may also be at higher risk due to increased difficulty with draining fluids properly through the skin's tissue layers.
Yes - understanding your risks and taking good care of yourself are two ways you can help reduce your chances of developing this condition. Avoiding injury or trauma to major lymph nodes — typically in neck/shoulder/arm areas- is advisable if possible. Making sure cuts/injuries in those areas heal quickly should also help minimize potential risks of developing secondary lymphedema down the line.
Additionally, avoiding obesity will help ensure proper circulation throughout all areas of your body; and caring for any underlying infections will go a long way towards preventing further issues concerning your circulatory system operating correctly within your body.
The most common lymphedema symptom is persistent swelling in an arm or leg that doesn't seem to subside. In addition to symptoms such as swelling, heaviness, and aching in the affected limb, there are several signs that may indicate the presence of lymphedema. These signs include:
The four stages of lymphedema are recurrent, hypertrophic, lipedemic, and fibrotic.
Recurrent lymphedema is characterized by chronic swelling of the affected area that worsens with time and generally requires treatment.
Hypertrophic lymphedema is marked by more consistent swelling that can become hard and red due to chronic inflammation and tissue damage caused by excessive accumulation of lymph fluid in the tissues.
Lipedemic lymphedema is a later stage where the skin shows signs of an abnormal fat deposition, including an orange peel-like texture and visible pores that look like pimples or goosebumps when touched.
Fibrotic lymphedema is the most severe type of Lymphedema and is associated with long-term scarring known as fibrosis, which may cause significant deformity if left untreated.
Yes - fortunately, there are many different forms of treatment available. Options vary depending on your situation, including manual lymphatic drainage, compression garments, bandaging, pumps, exercise, and skincare. In some cases, surgery or topical medications may also be used.
There are several self-care strategies that you can follow depending on your situation and the severity of your condition.
There may not be a fix-all treatment for lymphedema, but that doesn’t mean you have to settle for discomfort. You can live a full and active lifestyle with help from a care team with expertise in lymphedema treatment. In addition to a proper diagnosis and treatment plan, it is vital to stay positive, seek support from family and friends, and experiment with ways to manage symptoms under the care and attention of a qualified lymphedema expert.
Take control of your health and get the answers you seek. Schedule a consultation with a lymphedema surgeon at The Institute of Advanced Reconstruction today.

%20after%20cancer%20treatment_.webp)