Summarize This Article:
Summarize This Article:

“The goal of our surgical procedure is to improve or alleviate the symptoms of lymphedema. The goal is to improve the intrinsic drainage of lymphatic fluid from the limb. We still believe the therapy portion (massage, compression garments) is very important, even post operatively.” Dr. AshinoffDr. Russell Ashinoff, a plastic and reconstructive surgeon at the Institute for Advanced Reconstruction, is quoted in the following Asbury Park Press article about lymphedema, a condition characterized by fluid retention and tissue swelling caused by lymphatic issues. Dr. Ashinoff is one of only a handful of surgeons performing a procedure to relieve and/or improve lymphedema symptoms. This article was also highlighted on the Lymphatic Education & Research Network.
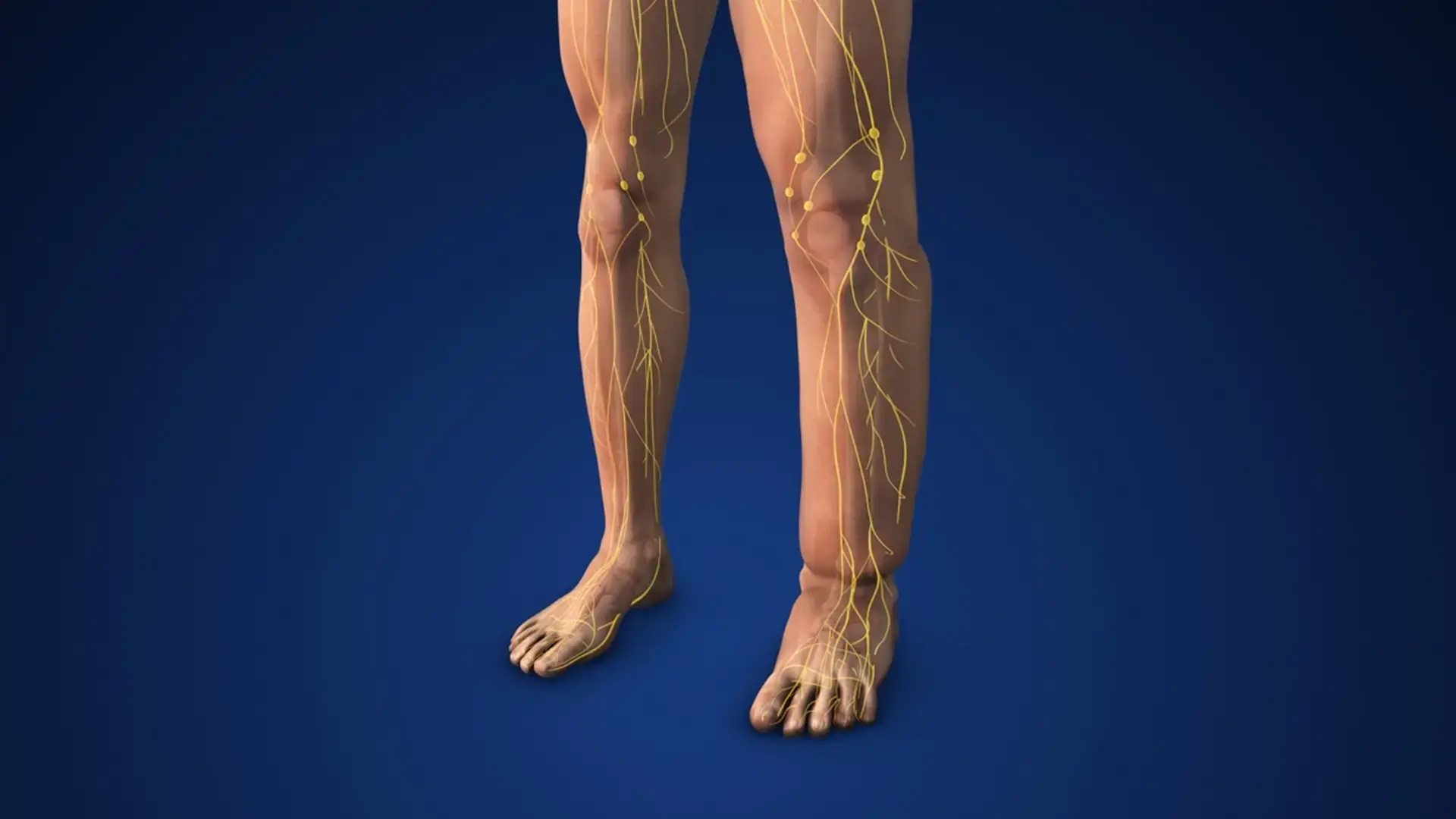
The lymphatic system is a critical component of the body’s vital and miraculous architecture. Its primary function is as a transportation system to the clear, colorless fluid, known as lymph, which contains the white blood cells that help clear toxins, waste, or other unwanted materials in every cell within the body. The lymph nodes, ranging from 500 to 700 in number, are the warriors of the immune system that help fight infection by filtering the fluid before it returns to the circulatory system. These nodes are found in large numbers in certain areas of the body, such as the groin, the neck, and the underarms.
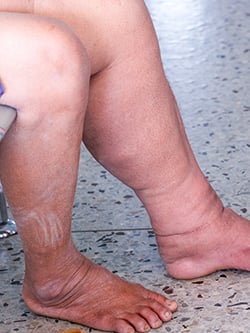
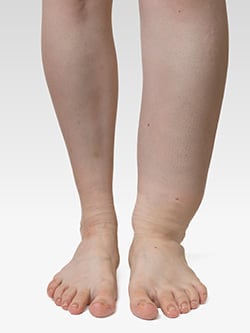
Lymphedema occurs when the lymphatic system is damaged or is not properly functioning. This can result in the accumulation of lymphatic fluid, chronic swelling, infections, and pain. It typically occurs in the limbs, although it can also affect the face, the neck, or the abdomen.
Lymphedema can be either primary or secondary. It can occur on its own (primary lymphedema), or it can be caused by another disease or condition (secondary lymphedema). Secondary lymphedema is often an undesirable byproduct of operations. Other causes include radiation, cancer, or infection. Secondary lymphedema is far more common in the populations of developed nations than primary lymphedema.
“Up to 10 million Americans have lymphedema and lymphatic diseases. That is more than AIDS, Parkinson’s disease, multiple sclerosis, muscular dystrophy, and ALS — combined,” according to William Repicci, Executive Director of the Lymphatic Education & Research Network.
The general medical community, however, is sadly uneducated about the lymphatic system and lymphedema, according to Stanley Rockson, MD, Director, Center for Lymphatic and Venous Disorders Stanford University Medical Center. He reports that in a four-year medical school education, half the physicians in North America heard about this incredibly important system for about a half-hour. A quarter of those medical school students receive only 15 minutes of instruction.
Lymphedema often occurs as a result of surgical lymph node removal. In order to determine if cancer has spread, surgeons may remove the lymph nodes in breast, ovarian, prostate, testicular, bladder, colon, and head and neck cancer, as well as melanoma. Although there are other causes for lymphedema, the majority of attention has been focused on patients who undergo breast cancer surgery. In breast cancer surgery, lymph nodes may be removed for evaluation from under the arm on the side of the affected breast, potentially resulting in lymphedema of that arm. Radiation is often delivered to this area as well, further increasing the chance that lymphedema will develop.
There is currently no cure for lymphedema. Yet, in addition to its physical toll, the psychological toll — including disfigurement, depression, and embarrassment — can significantly affect both one’s life as well as treatment.
Currently, lymphedema is mainly treated with Complete Decongestive Therapy (CDT), compression bandaging, and compression garments. Experienced therapists perform these treatments, and educate patients on self-care.
Relatively new and cutting-edge procedures, however, are providing new hope for lymphedema sufferers. A small number of specially trained reconstructive plastic surgeons perform Vascularized Lymph Node Transfer (VLNT), which uses advanced microsurgical techniques to take healthy lymph nodes from a low-risk location elsewhere in the body and transfer them to the affected limb, resulting in an improvement in limb swelling and decrease in infection rate in most patients. Lymphovenous bypass, a procedure to reroute the lymphatic channels into functioning veins, is also an advanced surgical treatment for lymphedema.
There are only a handful of surgeons treating the condition. Dr. Russell Ashinoff of The Institute for Advanced Reconstruction in New Jersey has been trained in the latest surgical procedures for lymphedema by pioneering surgeons in Europe. Dr. Ashinoff evaluates potential surgical candidates, both men and women, who have lymphedema because of a variety of causes.
According to Dr. Ashinoff: “The goal of our surgical procedure is to improve or alleviate the symptoms of lymphedema. The goal is to improve the intrinsic drainage of lymphatic fluid from the limb. We still believe the therapy portion (massage, compression garments) is very important, even postoperatively.” In performing these operations, Dr. Ashinoff uses the latest innovations, such as reverse lymph node mapping to determine the safest nodes to transfer, and advanced SPY imaging, which allows microsurgeons a real-time, clear view of microvessels, tissue, and organs.
Get educated: Learn about risk-reduction practices — before lymphedema becomes an issue in your life. In addition, if you receive a diagnosis of cancer, inquire about being evaluated for lymphedema risk before surgery. If lymphedema does become an issue, early diagnosis and treatment are critical.
Maintain a healthy weight and exercise: Obesity increases the risk of lymphedema.
And some studies have shown that breast cancer-related lymphedema may improve with weight loss in overweight people. A specialized exercise routine can be prescribed by an experienced lymphedema therapist.
Seek medical treatment: Ask your healthcare professional or contact lymphedema organizations online, which can provide a reference to a local lymphedema clinic where you can be evaluated by a certified lymphedema therapist. The therapist treats you, as well as teaches self-care to manage on a day-to-day basis.
The Lymphatic Education & Research Network is at the forefront of heightening awareness of these diseases and financing research for improved diagnosis, treatments, and, someday, a cure. In those efforts, several live-streamed symposiums are available on its website (lymphaticnetwork.org, under News and Events), featuring innovative treatments, including lymph node transplant surgery.

%20after%20cancer%20treatment_.webp)