Summarize This Article:
Summarize This Article:

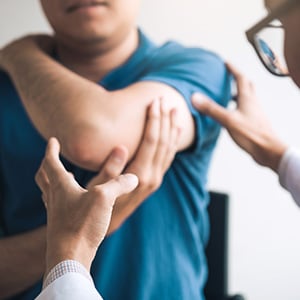
Yelena Shrayfel joins a long line of patients who have successfully undergone surgery for brachial plexus injuries with Dr. Andrew Elkwood of The Institute for Advanced Reconstruction. The 49-year-old avid motorcyclist incurred an injury due to an accident while riding in late 2012. Along with her shoulder and clavicle fracture, she severely injured her brachial plexus, causing the complete loss of function in her entire arm.
Within approximately six months following surgery (April 13, 2013), Shrayfel went from severe pain and no use of her arm to essentially complete function. In fact, she’s back riding her motorcycle. Another recent patient, a 9-year-old from Kenya, who made the trip to Shrewsbury, New Jersey, for surgery with Dr. Elkwood, had sustained a brachial plexus injury at birth. According to the American Academy of Orthopaedic Surgeons (AAOS), one or two of every 1,000 babies have brachial plexus injuries at birth, called Erb’s palsy, which results in arm weakness and loss of motion. This brachial plexus injury is often caused when an infant’s neck is stretched to the side during a difficult delivery. Dr. Elkwood successfully operated on the girl in October 2013.
Dr. Elkwood has been performing brachial plexus surgery for close to 20 years, treating patients who come to The Institute for Advanced Reconstruction from all over the United States and various countries around the world. The difficulty in determining the best treatment is a result of the complicated anatomy of this particular injury, as the brachial plexus is a network of intertwined nerves which run from the spine, into the neck, and into the arm.
“Part of the overall approach to brachial plexus treatment is based on the fact these injuries can be very complicated. They don’t often follow “textbook” cases. There are a lot of complicated issues,” stated Dr. Elkwood.
Frequently patients get somewhat better with time, but the extent to which they improve is unclear. As in many of the practice’s cases, the doctors hear this common lament from patients who are told by consulting doctors in a variety of specialties: “That’s all the healing you’re going to get.” The issue in these cases is that the complicated nerve network along the entire arm includes junctures in which the nerve swells and remains inflamed, thus eroding function. In the case of Shrayfel, Dr. Elkwood judged that surgical nerve decompression in multiple locations was warranted, and in this case, he was successful in returning function to the patient’s arm to a remarkable degree.
As Dr. Elkwood explains it, “The real trick is to aim for return of maximum function, which is done with a combination of a conservative approach with aggressive management and a good dose of judgment.”