DIEP flap reconstruction is the gold standard in autologous breast reconstruction, delivering a permanent, natural breast built from your own body by our reconstructive microsurgeons.
DIEP Flap Breast Reconstruction
Feel Like Yourself Again
What is DIEP Flap Reconstruction Surgery?
When breast cancer requires the removal of a large portion or one or both breasts, or the entire breast, reconstruction rebuilds the breast mound to look and feel as natural as possible.. The DIEP flap, short for Deep Inferior Epigastric Perforator flap, is an advanced technique available for rebuilding the breast using your own tissue. It is widely considered the gold standard in autologous breast reconstruction.
In a DIEP flap procedure, skin and fat are taken from your lower abdomen—the same area addressed in a tummy tuck—and carefully transferred to your chest to form a new breast. Your abdominal muscles are left intact. Muscle is neither moved nor removed.
The procedure is performed by microsurgeons who reconnect tiny blood vessels under a microscope to ensure the transferred tissue survives and thrives. This level of precision is not available everywhere. DIEP flap surgery is among the most technically demanding procedures in reconstructive surgery, and outcomes are directly tied to surgeon experience and center expertise.
Why Do Women Choose DIEP Flap Surgery?
The DIEP flap offers something no implant can: a soft, warm, and permanent breast built from your own living tissue.
The transferred tissue becomes a natural part of your body, so it moves and changes with you over time. It does not harden, rupture, or require replacement. Since no abdominal muscle is used, you are far less likely to experience the abdominal weakness, bulge, or hernia associated with older techniques like the TRAM flap. Additional benefits include a flatter abdomen from the donor site and the option to restore sensation to the reconstructed breast through nerve repair during surgery.
For women who will need radiation as part of their cancer treatment, autologous reconstruction holds a significant advantage. While radiation can damage implants, your own tissue is far more resilient. Multiple large studies consistently show that women who choose reconstruction with their own tissue report greater satisfaction with their results and better quality of life over the long term, compared to those who choose implants.
Planning Your Surgery
What Happens During Surgery
- Fat grafting: A minor outpatient procedure in which small amounts of your own fat are injected to refine the shape, smooth contours, or improve tissue quality, which can be particularly helpful in areas affected by radiation.
- Nipple reconstruction: If your mastectomy removed the nipple, it can be recreated using a minor local procedure performed a few months after your reconstruction has fully settled.
- Areolar tattooing: Highly realistic 3D medical tattooing restores natural color and appearance to the nipple-areola area with no additional surgery required.
- Lymphedema prevention or treatment: Women who undergo axillary lymph node dissection face a significant lifetime risk of lymphedema, chronic arm swelling that can affect comfort and function. During your DIEP flap surgery, our team can incorporate lymphatic procedures to reduce this risk or treat existing lymphedema, addressing both concerns in a single operation. Ask your surgeon whether you may be a candidate.
- Post-Mastectomy Pain Syndrome: Some women experience chronic nerve-related pain, numbness, or sensitivity after mastectomy or reconstruction. During revision surgery, targeted nerve procedures can help relieve discomfort and restore sensation by addressing injured or entrapped nerves, providing lasting improvement in quality of life.
Restoring Sensation
What Should I Expect After DIEP Flap Surgery?
Your Hospital Stay
After surgery, you will spend 2–4 days in the hospital, where your care team will closely monitor your reconstructed breast to ensure healthy blood flow to the new tissue. This monitoring is a routine and important part of your recovery, and you will be well supported throughout.
Recovery After Surgery
Remember that your body will be healing in two separate places—your reconstructed breasts and the site of the donor tissue. Recovery time from DIEP flap surgery is generally around 4-8 weeks, at which point most people can resume normal activity.
How Painful is DIEP Flap Surgery?
You may feel tired and sore for several weeks following your DIEP flap, as you would with any significant surgery. The good news is that DIEP flap tends to be less painful than other types of abdominal surgeries since it doesn’t involve moving or removing muscle. Be patient with your recovery, and be sure to slow down and rest if you experience pain.
What to Wear After Surgery
After DIEP flap surgery, you will want to wear comfortable clothing that is loose-fitting so it doesn’t irritate your incisions. Clothes that are easy to get on and off are ideal. You may be asked to wear a compression garment or girdle to support your abdomen. For your breasts, we recommend a surgical bra immediately after surgery, followed by a comfortable support bra as you continue to heal.
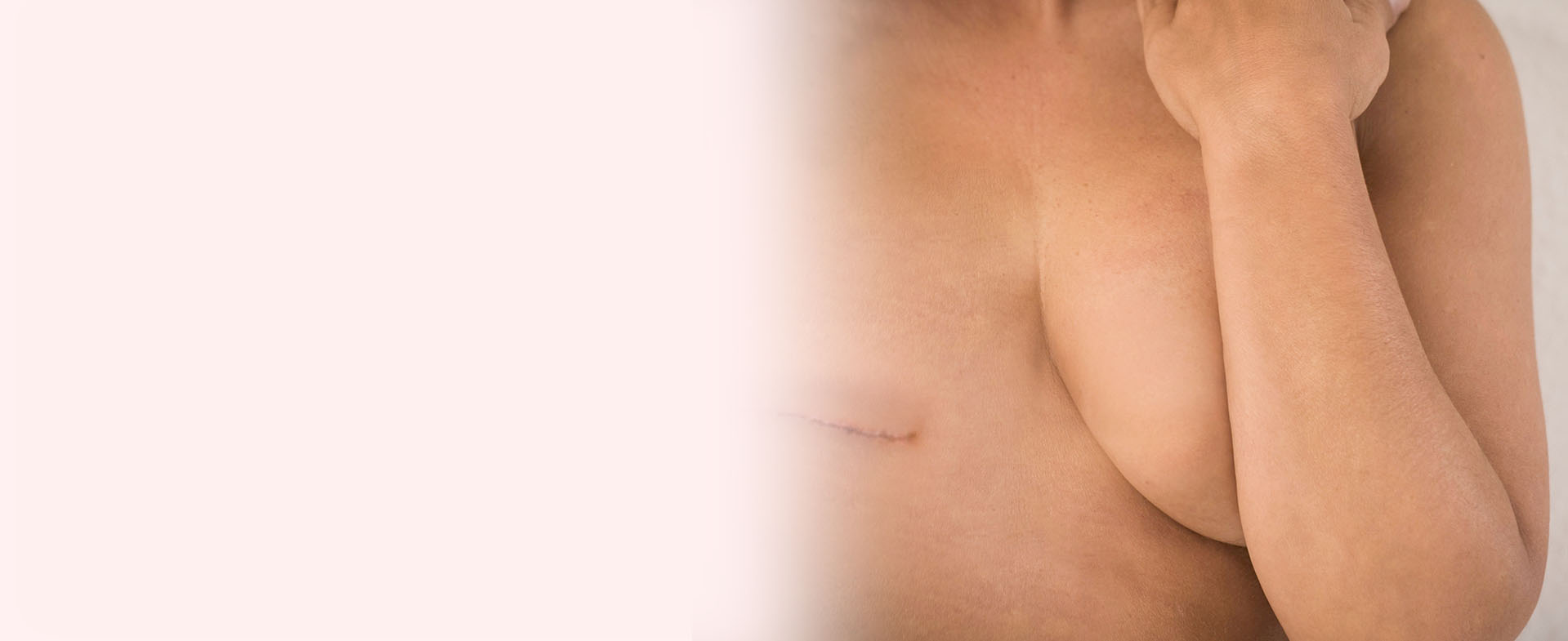
Will I Have a Scar?
The incision for DIEP flap surgery runs from hip to hip along the bikini line, and it will leave a mark that is similar to a tummy tuck scar. It could take up to a year for your scars to fade and the tissue to completely heal. It is important to follow your doctor’s care recommendations to ensure the best results.
How Does DIEP Flap Surgery Pair with Implant-Based Reconstruction?
For some women, abdominal tissue alone may not provide enough volume to achieve the desired breast size. In these cases, a DIEP flap can be combined with an implant, giving you the natural feel and durability of your own tissue while achieving the fullness you're looking for.
This combined approach also reduces the risk of implant-related complications, as the flap provides additional tissue coverage over the implant. Your surgeon will discuss whether this option is right for your anatomy and goals during your consultation.
Am I a candidate?
- Have adequate tissue in your lower abdomen
- Are in reasonably good overall health
- Do not smoke, or are willing to stop smoking well before surgery
- Have not had prior abdominal surgery that affected the key blood vessels; this is why pre-operative imaging is so important
Contact Us Today
Why Expertise Matters
DIEP flap surgery requires a level of training and institutional support that is not available at every hospital or plastic surgery practice. Our microsurgeons work within a dedicated program that provides the equipment, monitoring protocols, and experienced nursing staff this procedure demands.

Find a DIEP Flap Surgeon in New Jersey
The Breast Center of New Jersey has locations all over the nation with expert surgeons ready to help you.

%201.svg)







-min.png)
.webp)























-1.jpeg)

