Birth Defects Q & A
World Birth Defects Day is observed on March 3rd. Birth defects, also known as congenital anomalies, congenital disorders, or congenital conditions, affect around 120,000 babies in the US per year. One of the most common congenital anomalies are babies born with a cleft lip or cleft palate, sometimes both. At the Institute of Advanced Reconstruction, craniofacial surgery is performed by surgeons who have completed specialized fellowships in craniofacial surgery.
Dr. Sean Herman, a plastic and reconstructive surgeon who specializes in cleft and craniofacial surgical procedures, answers some questions about craniofacial surgery and discusses his video in the below video.
A: Craniofacial surgery is a surgical subspecialty of plastic surgery that addresses deformities of the head, skull, face, or jaw that are present at birth or develop later in life. The most common facial abnormalities include cleft lip with or without cleft palate.
Q: What is cleft lip surgery, and what does it involve?
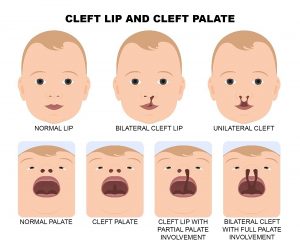
A: Cleft lip surgery is usually performed between 3 and 6 months of age. The procedure involves the closure of the lip and alveolar (gum ridge) defect. Cleft lip surgery repositions the upper lip and nose, which will allow the child to feed better while also helping to guide the growth of the maxilla, which is the bone that forms the upper jaw.
Q: What is cleft palate surgery, and what does it involve?
A: Cleft palate surgery is usually performed a little later in a child’s life, typically around the time they are one year old. The timing of the procedure is critical for speech development, as well as improving feeding. Cleft palate surgery, involves the closure of the nasal and palatal lining (mucosa) and the repositioning of the levator muscle (the muscle that lifts the palate for speech and swallowing purposes).
Q: How did you become interested in performing these surgeries?
A: I initially became interested in cleft and craniofacial surgery during my training, when I really saw how much of a difference these interventions could make in both the child’s and family’s life, giving them a chance to be just like any other kid. Hearing that your child needs surgery is never easy to digest, but knowing that both your surgeon and the team he or she works with are all well trained, and only have your child’s best interest at heart is always paramount.
Q: What advice would you give a parent whose child has to have craniofacial surgery?
A: There are many resources out there, such as those put out by the American Cleft Palate and Craniofacial Association, that may be of interest, so take time to look at some of these beforehand and discuss any questions you have with your surgeon or the team they work with, as well as the other providers in your child’s care, are the most important in the preoperative period. This way, all your questions are answered, and everyone is on the same page and understanding both the operative course and the postoperative recovery.
Q: What do you hope for the future of craniofacial surgery?
A: With recent advances in surgical techniques and devices, I hope the future of craniofacial surgery is able to deliver improved care with better outcomes by means of less invasive procedures with shorter recoveries and optimized results.