Occipital neuralgia is a nerve-induced headache similar to — and often confused for — a migraine. The occipital nerves run from the spinal column through the neck, up to the scalp at the back of the head. When these nerves are compressed, irritated, injured, or pinched by overly tight neck muscles, the result can be an occipital neuralgia headache.
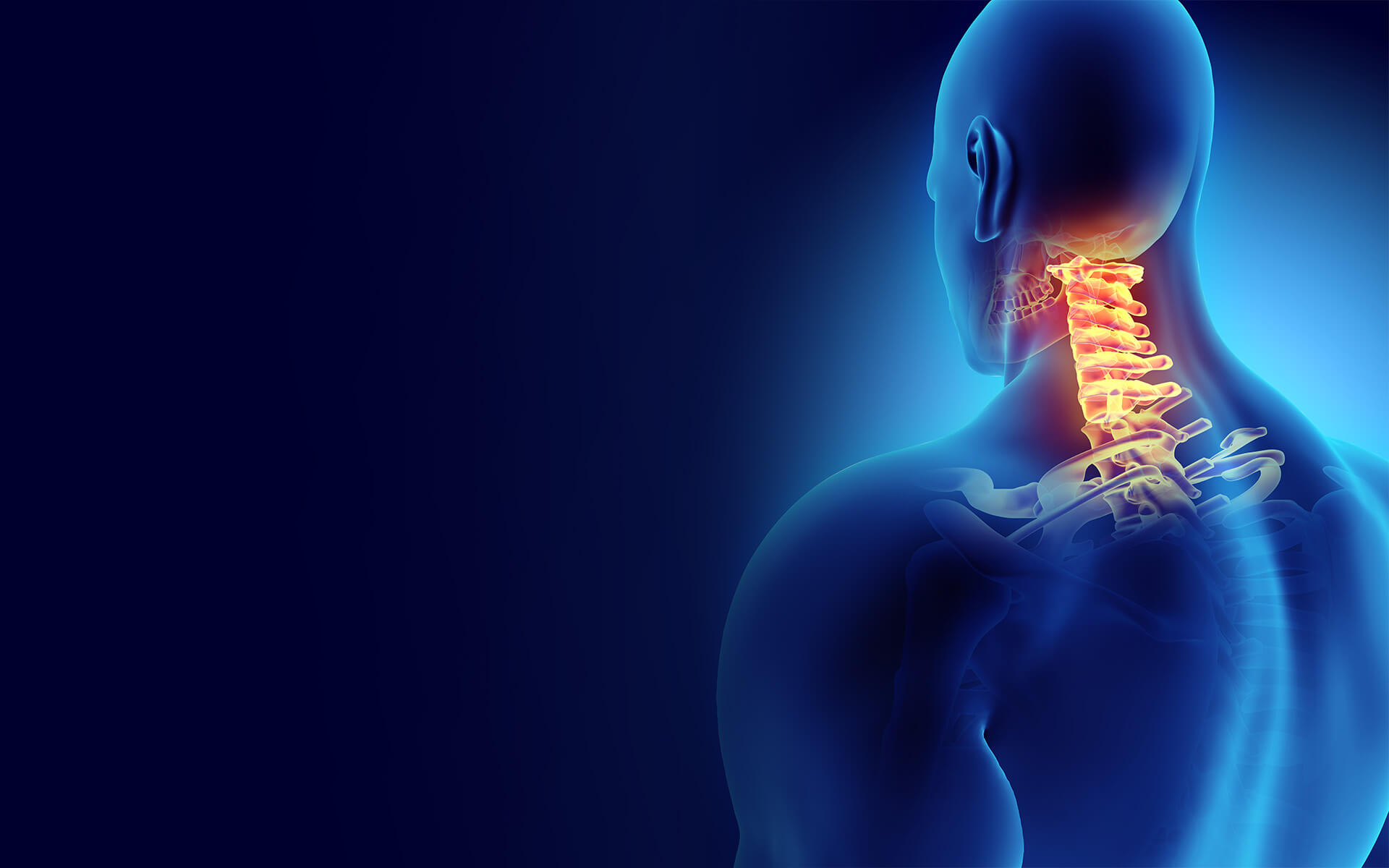
Understanding Occipital Neuralgia & Nerve Induced Headaches

What is Occipital Neuralgia?
Symptoms
Symptoms of occipital neuralgia include:
- Pain that begins in your neck and travels up to your scalp
- Aching, burning, or throbbing from the base of your head
- Sharp, shock-like, or piercing pain in your upper neck and back of the head
- Pain on one side of the head
- Pain behind your eyes
- Tender or painful scalp
- Pain when moving your neck
Causes
While occipital neuralgia and migraines share similar symptoms, such as sharp, piercing, and throbbing pain, their causes are very different. Occipital neuralgia occurs when nerves from the neck, back, and head get compressed or irritated.
Risk Factors
Some factors that may increase the risk of developing occipital neuralgia include:
- Previous head or neck injury: Trauma to the head or neck, such as a car accident or sports injury, can damage the occipital nerves and increase the risk of occipital neuralgia.
- Chronic tension headaches: People who suffer from chronic tension headaches may be more prone to developing occipital neuralgia.
- Poor posture: Poor posture, especially when it involves tilting the head forward for extended periods of time, can put strain on the neck muscles and occipital nerves, increasing the risk of occipital neuralgia.
- Aging: As we age, the muscles and soft tissues in the neck can become weaker and more susceptible to injury, increasing the risk of occipital neuralgia.
- Certain medical conditions: Certain medical conditions, such as rheumatoid arthritis and multiple sclerosis, can cause inflammation and damage to the nerves, including the occipital nerves, and increase the risk of occipital neuralgia.
It's important to note that these are just some of the factors that may increase the risk of developing occipital neuralgia. It's always a good idea to discuss any concerns about your health with a healthcare provider.
Diagnosing Occipital Neuralgia
Because occipital neuralgia has similar symptoms to a migraine, your medical professional will diagnose you based on the following:
- Patient history: headaches that begin in the back and travel up to the spine are correlated with occipital neuralgia, while migraines are often accompanied by visual disturbances and other pre-headache symptoms.
- Physical exam: Pressing on the occipital nerves on the base of the skull may elicit a negative response.
- Anesthetic nerve block: if you have a positive response (loss of pain) under an anesthetic nerve block, an occipital neuralgia diagnosis is likely to be made.
Occipital Neuralgia Treatments & Migraine Surgery
Occipital neuralgia is not a life-threatening condition, and many patients will recover from at-home occipital neuralgia treatments including:
- Heat or massage to soothe tight neck muscles
- Oral anti-inflammatory medications
- Prescription muscle relaxants
If occipital neuralgia symptoms do not improve with conservative treatments, your doctor may recommend minimally invasive or surgical procedures commonly used for migraine headaches treatment.
Nerve Blocks
A pain specialist may perform an outpatient procedure known as an occipital nerve block. Using a combination of local anesthetic and steroids, the nerve block is injected into the areas around the irritated nerve to provide pain relief lasting from several weeks to several months. In many cases, the pain will not return, while in others, subsequent treatment may be required.
Botox for Headaches
Another treatment for occipital neuralgia involves Botox injections, a common approach to migraine headaches treatment. Botox is a form of neurotoxin produced by the bacteria that causes botulism. When it is injected near the nerve endings involved in headaches, it can interfere with pain signals sent to the brain.
Nerve Decompression Migraine Surgery
Surgery is another option for occipital neuralgia and migraine headaches treatment that can permanently reduce or relieve pain. Nerve decompression surgery is a minimally invasive procedure targeting nerves in the neck and head region. The surgeon will remove muscle, blood vessels, and tissue lining that affect nerve function. Multiple trigger points can be addressed in one procedure. Nerve decompression migraine surgery is typically an outpatient procedure done under general anesthesia that takes 2 to 3 hours to complete. Recovery can take up to two weeks.
Our Doctors
The Institute for Advanced Reconstruction is one of the few places in the country offering advanced treatments for occipital neuralgia, including nerve decompression surgery. We’ve been successfully treating occipital neuralgia and migraine headaches since 2005.
Patient Stories
Migraine Surgery Near Me
Insurance Information
The Institute for Advanced Reconstruction participates in a wide range of insurance plans, including those listed below. However, each physician has their own accepted insurance and hospital affiliations. Before scheduling an appointment, please contact your insurance carrier to confirm that your provider is in-network.
If we are not an in-network provider, our friendly insurance specialists will help you find the most coverage available for your treatment.
- Horizon Blue Cross Blue Shield of New Jersey
- Medicare
- Railroad Medicare
- Aetna
- Cigna
- United Healthcare
- Oxford (Freedom, Liberty)
- MagnaCare
Related Videos
Patient Resources
Am I a candidate for migraine surgery?
Stop headache pain before it stops you. Schedule an appointment today to find out if our occipital neuralgia treatments are the right solution for your head and neck pain.






.jpg)